Preface: About 1 year ago I began thinking about ways to improve non invasive intensity threshold estimation. After all, even though gas exchange is great, most of us don't have easy access to this on a regular basis and thus rely on "surrogate" methods. It occurred to me that combining two different threshold estimations (one being DFA a1 HRVT) into a single "Combo" value could potentially lead to a better personalized agreement with gold standard measures. I discussed this idea with a leading exercise physiology group and it was decided to give this concept a go. Unfortunately, it took longer to perform, analyze, write and submit than anticipated and that study is still in peer review (let's call it "Study #1"). However, fast forward 8 months to the completion of our Kubios Respiratory Rate validation project. As we discussed in that report, a prior publication did show reasonable agreement of respiratory rate thresholds to gas exchange values. With that in mind, I decided to repeat their methodology with our Kubios EDR data and both validate the EDRT concept as well look at whether the "Combo" result (with DFA a1), yielded better agreement to gold standards. Therefore, even though the current article/post should be labeled "Study #2" in dealing with threshold combinations, due to the issues of peer review and journal timelines, it's out first.
Introduction:
Exercise intensity thresholds are often discussed in terms of their importance for both training distribution, comparisons of fitness and athletic status. However despite knowing the particular heart rate, power or speed at the first or second threshold, we sometimes forget that some these metrics are really not that precise. When we compare things like HRVTs, FTPs, Crit power, muscle desat breakpoints to their corresponding gold standards, the group averages look fairly close but the individual values can vary quite a bit. Since exercise in an inappropriate zone can have adverse consequence, we should be thinking about how to do better with this estimation. After looking at some of my own noninvasive threshold testing data, I came up with the following idea - why don't we use two disparate threshold measuring paradigms, then average the results for a "Combo" threshold. For instance, let's say that during an incremental cycling ramp my a1 HRVT2 came out to be 148 bpm, but by NIRS breakpoint analysis (muscle O2 desat) it was 158 bpm. My idea was to simply split the difference - designating the "Combo threshold" at 153 bpm. The idea is if a single modality is incorrect, the combo value would be partially corrected by the more precise method (whichever one that is). If they agree, then great, but if not, at least the mean value will be closer to the truth. Obviously, if both thresholds are incorrect, we are still left with an incorrect figure, but since "on average", the group means are usually close, the core concept should still be sound.
ECG derived respiratory rate thresholds - EDRT:
As previously reviewed, Kubios HRV software derived respiratory rate is capable of matching up against gas exchange through an exercise ramp. As I was reading the background information regarding respiratory rate exercise related applications, one in particular caught my interest - respiratory rate intensity threshold assessment. As we discussed in our article, Cross et al showed that after some "data processing", the respiratory rate can be used to derive two intensity thresholds signifying VT1 and VT2. Unfortunately, the "data processing" was (to me) out of my skill set at the time. The methodology entails creating a 6th order polynomial curve using the raw resp rate, then taking the second derivative of that curve. The second derivative curve (over time) should possess 2 maximal points that correspond to AeT and AnT thresholds (VT1, VT2). Being one of those types who doesn't like to give up, I gradually chipped away at this problem and eventually found a way to solve it. From this point on I'm going to use the term EDR (ECG derived resp rate) instead of resp rate - but if you have another source of resp rate data (Hexoskin, other wearable, gas exchange etc), that data may also be used. I will warn you that non Kubios HRV (Garmin, alphaHRV) sources may not be precise or reliable enough to run this calculation. Even Kubios resp rate derived from RR intervals (not ECG) is unpredictable in terms of accuracy (see figure 3 here).
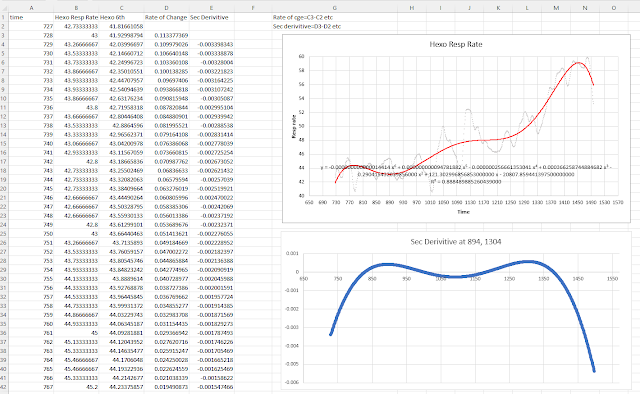
The first part of the "data processing" is not particularly difficult. Here we need to plot the resp rate over time, then use Excel to apply a trendline. The trendline is going to be that 6th order polynomial mentioned above. The real hurdle is getting the data points for each increment of time. In other words, we have our column of raw data (resp rate) and we need to get the corresponding sequence of "smoothed" data that is represented by the 6th order trendline. It turns out that one can put the trendline equation into the Excel cell, but one needs to reformat the equation to a numeric rather than text.
So, we now have a set of "smoothed" EDR over time (the trendline values) - but how do we get the second derivative of this data series. In simplistic terms, the first derivative is just the difference between one value (rows) and the next over time (velocity) and the second derivative is the difference in the first derivative over time (acceleration). If we keep this in mind, then plotting this out in Excel becomes easy.
Below is the supplemental file from our publication outlining how to do this, step by step:
The end result to the above tutorial is that you will have obtained a first and second EDRT.
As another example of this process, below is my worksheet for the respiratory derived thresholds using the Hexoskin. This illustrates the ability of the 6th order smoothing technique to actually produce reasonable results despite significant point to point variation.
The light gray is the raw Hexoskin data (which is not smooth) but the trendline is workable and produces a proper two maxima second derivative.
My EDR smoothed curve using the Movesense ECG was virtually identical but without the highly variable raw data bounce:
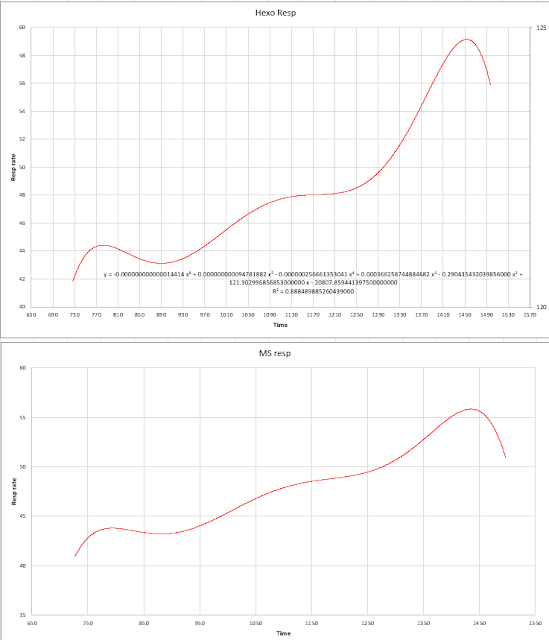 |
| Smoothed Hexoskin and Movesense EDR over time |
The time of each maxima can be paired up with either HR or power (if the ramp slope is not too steep).
In this case the EDRT1 was 137 bpm and the EDRT2 was 162 bpm.
The HRVT calculation was similar:
These are close to my lactate and gas exchange values but the important point is that there are now two "concepts" supporting my guesstimate as to intensity thresholds.
Summary Points so far:
- Combining 2 (or more) threshold surrogate concepts makes sense on multiple levels.
- If one of the metrics is unable to be obtained, the remaining marker may be adequate for delineation.
- To obtain an EDRT, an incremental ramp to failure is needed. Although this is not ideal, it's not a total deal breaker.
- On the other hand, as we have shown in other post and articles, the HRVTs can be estimated from constant power intervals, sub maximal ramp or step tests.
What is the cost of doing a double threshold estimation as above?
For a single HRVT (DFA a1) calculation, the cost is near zero - if you already have a Polar H10. In this case recording the RRs, uploading to Runalyze, AIEndurance or using Fatmaxxer (or other apps) gets you pretty close to Kubios accuracy.
However for the EDRT we need the ECG tracing and Kubios Premium/Scientific to accurately measure respiratory rates. What about using just Garmin HRV or alphaHRV app for our respiratory rates? As I've pointed out (and as seen in the Sensors study), RR timing derived respiratory rates may not be precise/consistent enough for this type of calculation (YMMV).
Which leaves us with this cost breakdown:
Kubios Scientific $380
plus the following options:
Movesense Medical about $220
Movesense HR+/HR2 about $100
Polar H10 about $85
Total about $465 to $600 depending on options
I will not make a value judgement here but considering what some other accessories of dubious merits cost (continuous glucose monitor, Core temp, hydration sensor etc), this seems well in the worthwhile range cost:benefit wise. Additionally, having continuous ECG recording and display (with Kubios) can potentially alert one to cardiac arrhythmia before it becomes an issue.
Precautions before testing:
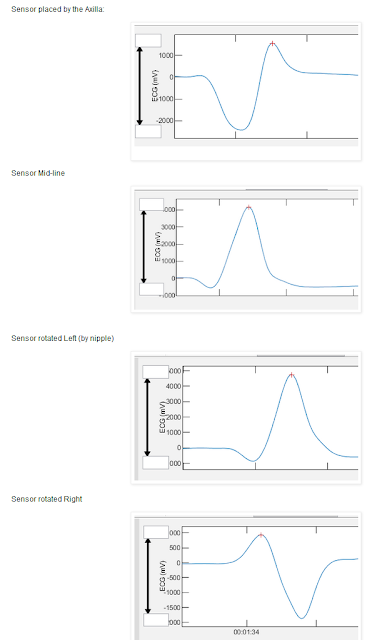
As I've discussed before, the signal strength and waveform of the HRM/ECG are critical for accurate representation of RR timing and hence DFA a1. Perhaps even more-so, this applies to EDR, where the R wave signal fluctuation is used to estimate respiratory frequency. In short, make sure you have positioned the module and belt to optimize signal strength before you run the test!
Summary:
- In this post, we introduce the concept of combining two disparate surrogate markers to better agree with an individual's "true" first and second intensity threshold.
- In the current case, the DFA a1 based HRVT was paired with a relatively unfamiliar surrogate, namely the ECG derived respiratory rate (EDRT).
- By themselves, decent agreement was seen with VT1 but was strongest at VT2 (RCP).
- The EDRT2 was surprisingly accurate in estimating VT2/RCP, making this a promising method for this important boundary.
- It is possible to get the second derivative of the 6th order polynomial of the respiratory rate purely use MS Excel (see supplement).
- The combined threshold (simply the average HR between the two) had closer agreement and less bias than each one separately.
- Both surrogates were able to be calculated with available hardware (Movesense Medical ECG) and software (Kubios Scientific) for a total projected cost of about $600.
- Make sure you look at the ECG waveform/voltage before testing. Move the HRM belt if needed.
- Study #1 has finally come out! - Combining NIRS and DFA a1 for critical intensity estimation
Heart rate variability during dynamic exercise
- Firstbeat VO2 estimation - valid or voodoo?
- Heart rate variability during exercise - threshold testing
- Exercise in the heat and VO2 max estimation
- DFA alpha1, HRV complexity and polarized training
- HRV artifact avoidance vs correction, getting it right the first time
- VT1 correlation to HRV indexes - revisited
- DFA a1 and Zone 1 limits - the effect of Kubios artifact correction
- HRV artifact effects on DFA a1 using alternate software
- A just published article on DFA a1 and Zone 1 demarcation
- DFA a1 vs intensity metrics via ramp vs constant power intervals
- DFA a1 decline with intensity, effect of elevated skin temperature
- Fractal Correlation Properties of Heart Rate Variability (DFA a1): A New Biomarker for Intensity Distribution in Endurance Exercise
- Movesense Medical ECG V2.0 Firmware brief review
- Movesense Medical ECG - improving the waveform and HRV accuracy
- DFA a1 and the aerobic threshold, video conference presentation
- DFA a1 - running ramp and sample rate observations with the Movesense ECG
- DFA a1 calculation - Kubios vs Python mini validation
- Frontiers in Physiology - Validation of DFA a1 as a marker of VT1
- Real time Aerobic thresholds and polarized training with HRV Logger
- Active Recovery with HRV Logger
- DFA a1 and exercise intensity FAQ
- DFA a1 agreement using Polar H10, ECG, HRV logger
- DFA a1 post HIT, and as marker of fatigue
- DFA a1 stability over longer exercise times
- DFA a1, Sample rates and Device quirks
- DFA a1 and the HRVT2 - VT2/LT2
- Low DFA a1 while running - a possible fix?
- Runalyze vs Kubios DFA a1 agreement
- DFA a1 - Runalyze vs Kubios vs Logger results in a cyclist
- Best practices for Runalyze and DFA a1 thresholds
- ACSM - HRVT validation in a cardiac disease population
- FatMaxxer - a new app for real time a1
- Another look at indoor exercise without a fan
- ECG artifact strips from Fatmaxxer - a guide
- ECG arrhythmia and artifact visualization tips
- DFA a1 as a marker of endurance exercise fatigue
- To train hard or not, that's the question
- DFA a1 HRVT and Ramp slope
- DFA a1 and optimal HRM belt position
- DFA a1 threshold in a cardiac population
- Rapid HRVT graphing and interpretation
- Atrial fibrillation - warning signs from chest belt recordings
- A tale of 2 HRVs - afib vs noise
- Pitfalls in DFA a1 - Polar belt position
- AlphaHRV - the first native Garmin DFA a1 data field
- HRVT validation in Elite Triathletes
- Recent podcast at Scientific Triathlon 3/22
- The DFA a1 App Matrix
- New - Review in Frontiers in Physiology
- Fitness Dashboard - initial review
- Respiratory Rate metrics, ECG vs HRV, Kubios vs Garmin
- Respiratory rate correlation to lactate during exercise
- Kubios Scientific and DFA a1 thresholds
- alphaHRV respiratory rate tracking vs Garmin/Kubios
- Combining NIRS and DFA a1 for critical intensity estimation
- A new paradigm for Intensity thresholds - combining surrogate markers
- Ramp slope and HRV thresholds

What about combining these two:
ReplyDeletehttps://www.fitnesshrv.com/ to record full ECG from Polar H10
https://neuropsychology.github.io/NeuroKit/examples/ecg_edr/ecg_edr.html?highlight=edr To make use of the amplitude change occurring in the ECG from a H10?
You could try using the H10. We have not validated it (as was done with the Movesense), but it might work just fine. The EDRT study we cited in the article did use the H10 with upsampling.
ReplyDeleteMay I suggest that you correct the units on your waveform pictures? The units should be µV and not mV. Or use the decimal points because this creates confusion for several people. An R-peak > 3000mV (=3V) is unrealistic.
ReplyDeleteHa, these are just default scaling units. If you are interested "1000" = .38 mV for the Movesense ECG.
ReplyDelete